资料与方法
一、对象
二、方法
结果
一、病理及随访结果
二、婴幼儿陈旧性卵巢囊肿蒂扭转的超声特征及诊断效能
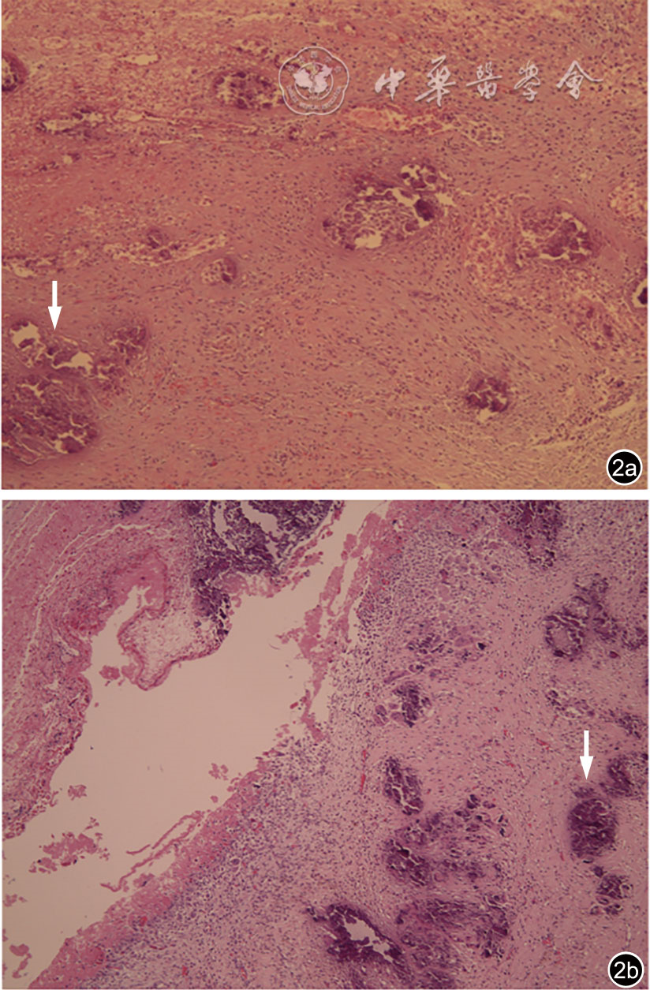
图1 婴幼儿陈旧性卵巢囊肿蒂扭转超声图像表现为钙化。图a为女性婴幼儿出生1个月,超声可见右侧腹囊性包块,内见液体分层征,囊壁可见散在环状钙化点(箭头所示),超声诊断右侧卵巢及囊肿陈旧性扭转坏死;图b为女性新生儿出生5 d,超声可见左侧腹囊实性包块,内见液体分层征,囊壁可见多发钙化斑(箭头所示),超声诊断左侧卵巢及囊肿陈旧性扭转坏死 |
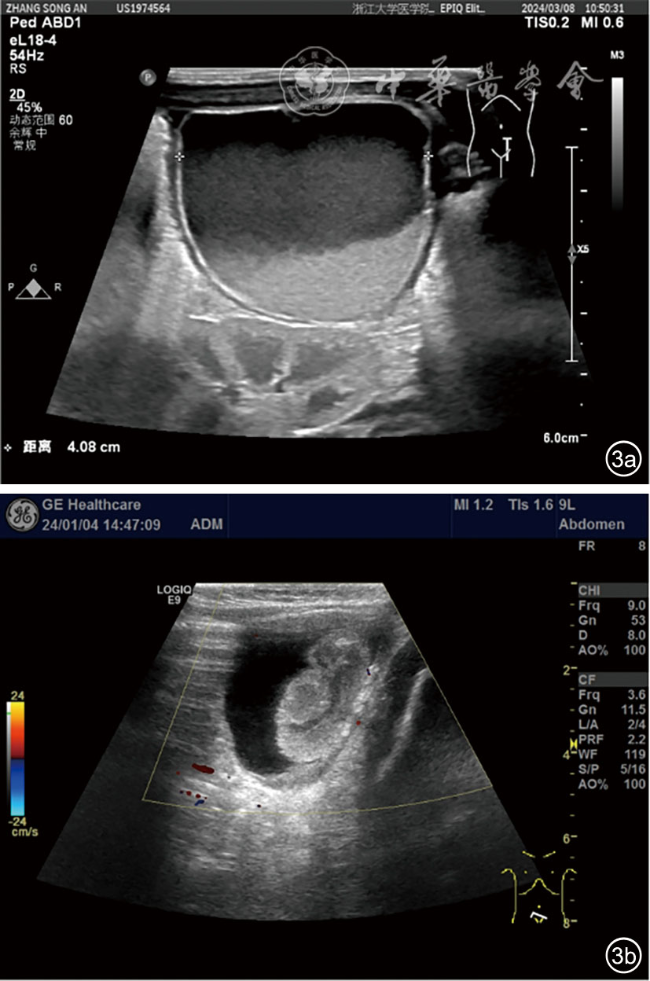
图3 婴幼儿陈旧性卵巢囊肿囊内分层超声图像。图a为女性婴幼儿,出生1个月,超声可见左下腹囊性包块,内见液体分层征,超声诊断左侧卵巢囊肿伴扭转;图b为女性婴幼儿,出生2个月,超声可见盆腔左侧囊实性包块,内见回缩样团块回声,囊壁可见斑片状钙化,超声诊断左侧卵巢来源囊肿及左侧卵巢陈旧性扭转坏死 |
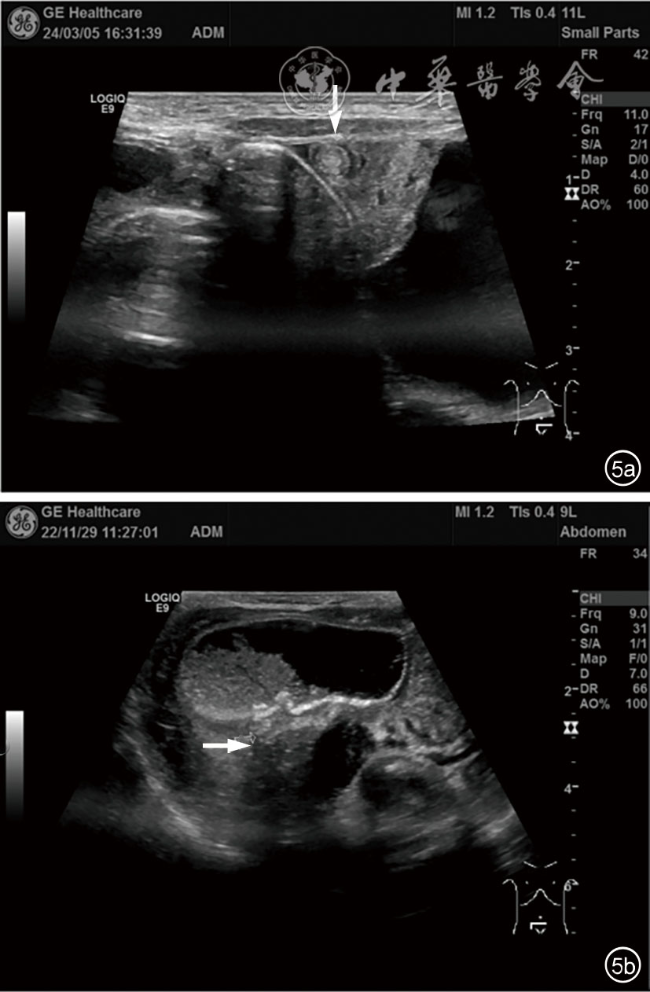
图5 婴幼儿陈旧性卵巢囊肿漩涡征样蒂结构超声图像。图a为女性新生儿,出生1 d,超声可见左中腹囊性包块,包块左下缘见螺旋样同心圆结构(箭头所示),扭转约360°,超声诊断左中腹囊性包块,左侧卵巢来源可能性大合并扭转考虑;图b为女性新生儿,出生8 d,超声可见右下腹囊性包块,内见液体分层征,包块后下缘低回声团,呈蒂样结构(箭头所示),超声诊断右侧卵巢来源囊肿及右侧卵巢陈旧性扭转坏死可能性大 |
三、陈旧性卵巢囊肿蒂扭转的超声诊断准确性
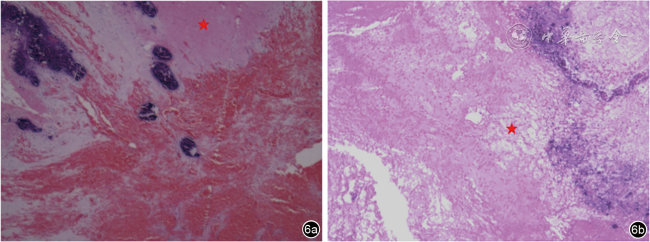
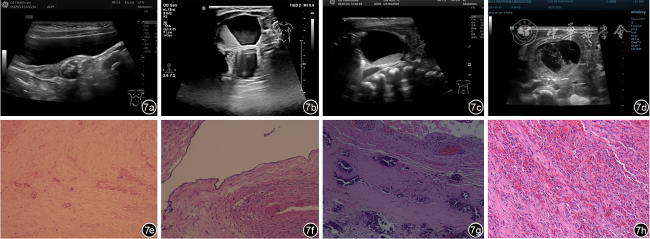
图7 陈旧性卵巢囊肿蒂扭转超声误诊病例超声及病理表现。图a为女性婴幼儿,出生12个月,超声可见盆腔内不均质团块回声,内见斑片状强回声伴声影,超声诊断左侧卵巢来源畸胎瘤;图b为女性婴幼儿,出生1个月,超声可见右侧附件区囊性包块,内见液体分层征,超声诊断右附件畸胎瘤;图c为女性新生儿,出生4 d,超声可见盆腔内囊实性包块,内见液体分层征,超声诊断盆腔囊实性包块,畸胎瘤待排;图d为女性新生儿,出生3 d,超声可见右侧腹囊性包块,内透声差,见分隔,超声诊断右侧腹囊性包块,肠重复畸形可能;图e(与图a为同一病例)病理提示左侧卵巢组织广泛坏死伴钙化改变,可见少许深蓝色团块状沉积和细胞核的碎裂消失(HE ×40);图f(与图b为同一病例)病理提示卵巢单纯性囊肿伴坏死钙化,可见散在细胞核的碎裂消失(HE ×100);图g(与图c为同一病例)病理提示卵巢囊肿蒂扭转伴坏死,可见深蓝色团块状沉积和红细胞在血管外聚集(HE ×200);图h(与图d为同一病例)病理提示卵巢囊肿蒂扭转伴出血坏死钙化,可见红细胞散在分布(HE ×200) |